Neurogenic genital pain is relatively rare and may affect between 0,001-1% of the population, and up to 4% of patients with prediagnosed chronic pelvic pain (Spinosa 2006). However, its true occurrence rate may be underestimated due to diagnostic difficulties. Most of these patients are sent to urology or gynecology consults, but obvious pathology is undetected. This will often warrant an electrodiagnostic study, but because these are notoriously unreliable in entrapment neuropathies (Rousseff 2004, Larsen & Chieng 2019), the results will either be negative or equivocal, confusing the patient and physician, both. The gold-standard diagnostic rule persists to be a diagnostic nerve block of the pudendal nerve, but because the nerve can be easily missed if the injection is done without ultrasound guidance, this is yet another pitfall for missed diagnosis.
Etiology
The cause of neurogenic genital pain is considered elusive, and the pathology idiopathic. Obvious causes such as iatrogenic damage (eg. surgical transection or partial neurotmesis), tumors or similar problems causing mechanical compression or derangement of the nervous networks must be excluded first. Systemic causes of neuropathies, such as MS, diabetes or hypovitaminosis should also be excluded, but are still not common causes of focal genital pain. As stated, however, most of these incidences are deemed idiopathic. Many believe that genito-local irritation of the pudendal nerves is what is causing the issues, and many undergo very painful intravaginal massage or similar horrible treatments with minimal improvements. Some also perform local entrapment-liberation of the pudendal nerves in the pelvic floor area itself, but the success rates are not staggering.
In reality, neurogenic genital pain is just a component, a symptom, of a larger underlying problem. Most if not all of these patients have widespread symptoms of neuropathy, consistent with lumbosacral plexus affection (Larsen & Chieng 2019). Concomitant pain along the cluneal, genitofemoral, lateral femoral cutaneous or saphenous nerves is very common. Pressure tests applied to these nerves will elicit abnormal amounts of pain.
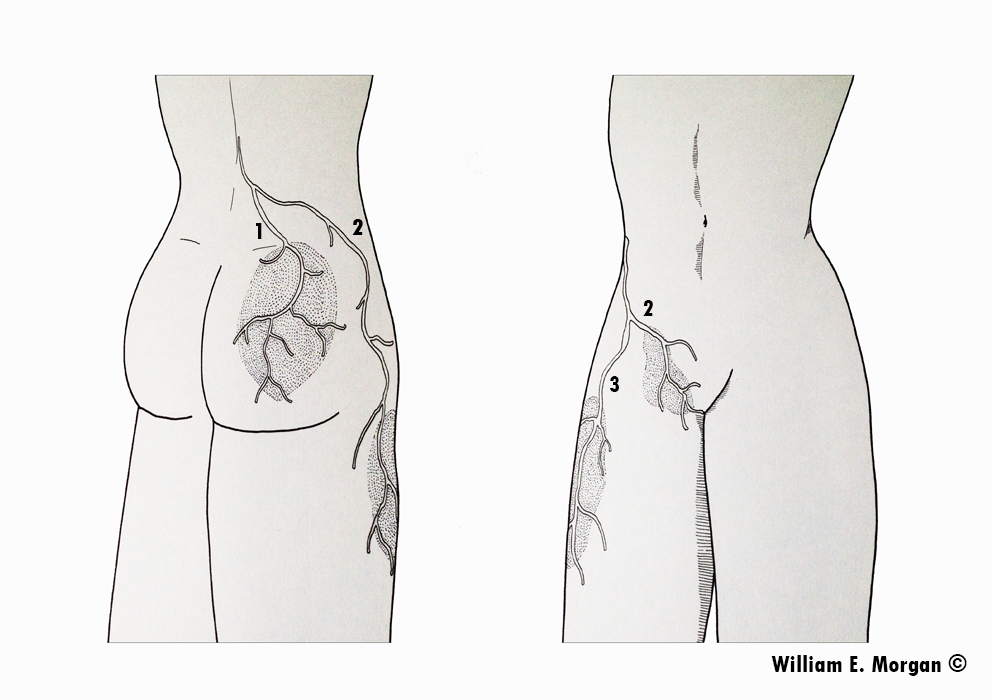
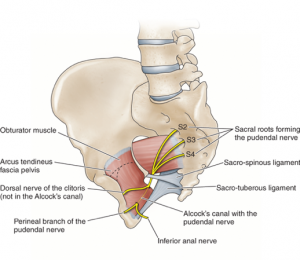
There are two main sources of genital pain, and which one it is, depends on the triggers that the patient has as well as whether or not it is centered or unilateral (it can also be bilateral). Pudendal neuralgia generally worsens when sitting and when loading the posterior hip muscles. It is not actually a genital problem, but it manifests distally (ie. where the nerve ends up). The pudendal nerve forms from the S2-4 nerve roots and emerges beneath the piriformis muscle, before it ventures into the Alcock’s canal between the obturator internus muscle and the falciform ligament. It is, in essence, a piriformis syndrome manifesting in your genitals. There are two pudendal nerves, each innervating the left and right hemispheres of the pelvic floor, rectum, perineum and vagina (or penis). Severe weakness of the deep hip rotators, including the piriformis and obturator muscles result in hyperfibrosis and thus loss of neural gliding in their fascial passages, which is the cause of the entrapment. This is curable in most circumstances with appropriate strengthening rehabilitation of these muscles.
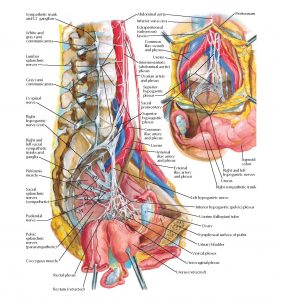
The other cause of neurogenic genital pain is inferior hypogastric entrapment plexopathy. The inferior hypogastric plexus is a part of the sympathetic nervous system and innervates your organs. It tends to cause a burning, electrical, cramp-like feeling in the anus, perineum and root of the penis or vaginal opening, or hypogastric type (“menstrual”) pains. The pain will be experienced as “central” in the pelvic floor, and tends to worsen with stretching of the psoas major, eg., when standing up from having being seated, walking, or running, especially uphill. The hypogastric plexus anastomoses with the somatic root ganglia of the lumbosacral plexuses. The piriformis muscle affects the sacral plexus (as it irritates the proximal sciatic/distal plexus), whereas the lumbar plexus is affected by the psoas major muscle as it literally pierces the psoas major as it emerges. This can co-affect the parallel sympathetic chain and thus also the hypogastric plexus, causing dysautonomia and sympathalgia. The lumbar plexus directly connects to the sacral plexus through its lumbosacral trunk, and this may also predispose (“sensitize”) due to the the double-crush phenomenon (Larsen & Chieng 2019). Again, as shown above for the sacral plexus, weakness of the psoas major results in restricted neural gliding through the myofascial of the psoas major muscle and consequent entrapment neuropathy. Gentle strengthening is the key strategy for amelioration.
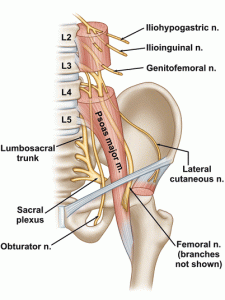
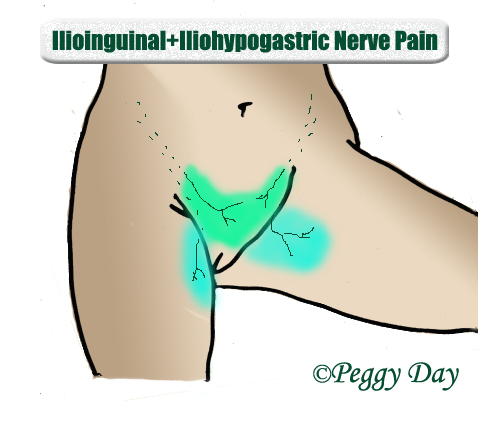
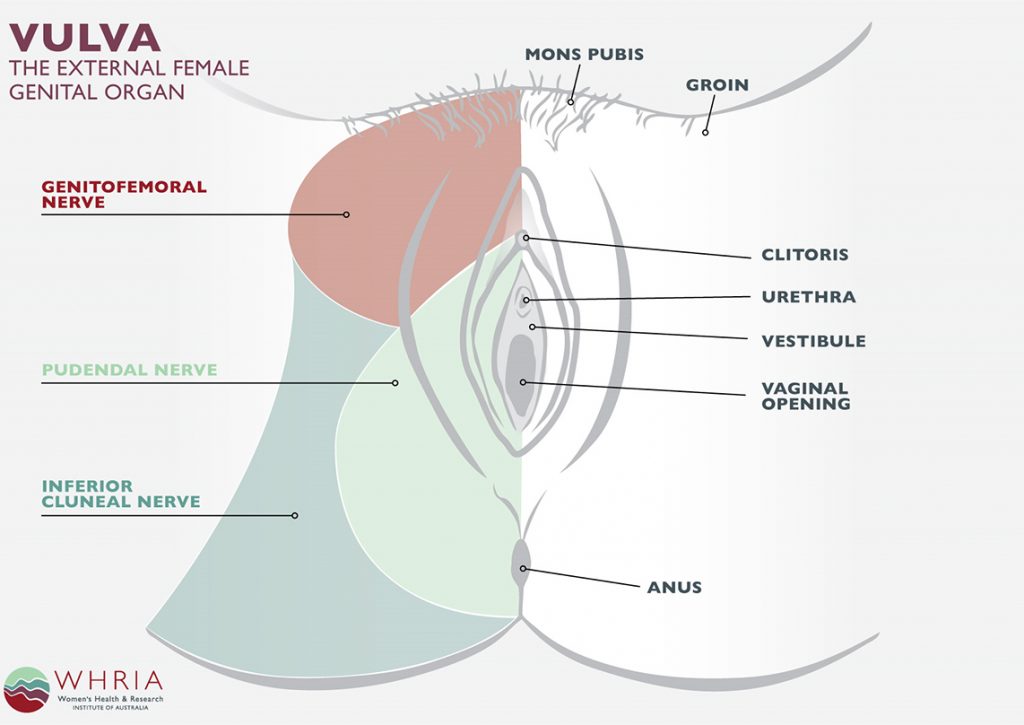
Anterior labial or testicular pain is usually caused by ilioinguinal or genitofemoral nerve entrapment. This, either due to entrapment of the very same nerves within the psoas major muscle or due to positional compression between the pectineus muscle and the inguinal ligament. This is caused by tight groin muscles and sitting too much leaning forward, excessive squat depth, etc. Posterior testicular pain is a symptom of pudendal neuralgia.
Stress, anxiety. Unfortunately, the vast majority of patients suffering from entrapment induced genital pain also suffer from stress and anxiety. This does not mean that their pain is not real, or that they are imaging the pain. It does, however, mean, that the muscular issues that are responsible for the entrapment neuropathies are grossly worsened, if not caused, by the patient’s stress levels. Reducing “tenseness” is a vital component in treating this problem and it must not be neglected. See the “muscle clencher” article on my website: mskneurology.com/chronic-muscle-clencher-woe-to-you. Do not underestimate the relationship between stress, body tension, and entrapment neuropathies.
I have also found patients who perform cycling or running sports to be especially predisposed for these problems, especially if they also suffer from anxiety disorder or high stress, PTSD, etc.
Diagnosis
Compatible symptomatology and exclusion of other causes are always the first important considerations. Gyn/urological examinations will be unremarkable or without detection of compatible pathology. MRI will not reveal masses or similar lesion of the lumbosacral plexuses, and serological workups for neuropathies will be normal. The patient will have mechanical triggers for their symptoms, such as sitting down over periods of time, standing up or walking, especially uphill or on stairs, and will have symptoms that fit with the neuroanatomy.
Most of these patients have concurrent hip impingement (as it is caused by weakness of the hip stabilizers and bracing of the external muscles). They may have hip-intracapsular effusions seen on MRI, and often labral tears. This is not the cause of the symptoms, just a passive sign of an underlying problem. If you’re lucky, inflammation of the piriformis or psoas tendons may be visible on the MRI, but this is not the norm. Hypointensity of the distal piriformis attachment is common, especially on PD FATSAT, but usually not reported as pathology.
Patients with pudendal neuralgia may have uni- or bilateral symptoms, usually worse on one side. They get worse when sitting, especially on hard surfaces. Sitting leaning forward (greater degree of hip flexion) makes it even worse, as this stretches the piriformis and obturator muscles. The pain may be localized in the penis or vagina, perineum, or rectum and medial buttock, on that side. There may also be numbness of the glans (head of the penis) or clitoris. Pain during intercourse is common, especially for women. Difficulty reaching orgasm may occur as well. In extreme circumstances, there may be weakness of the anal sphincter, but this is not the normal. Electrodiagnostic tests are almost always normal. However, a well-placed ultrasound-guided nerve block will generally be positive, confirming the diagnosis. Strengthening the piriformis and obturator muscles, and with this developing worsening of symptoms, also confirms the diagnosis.
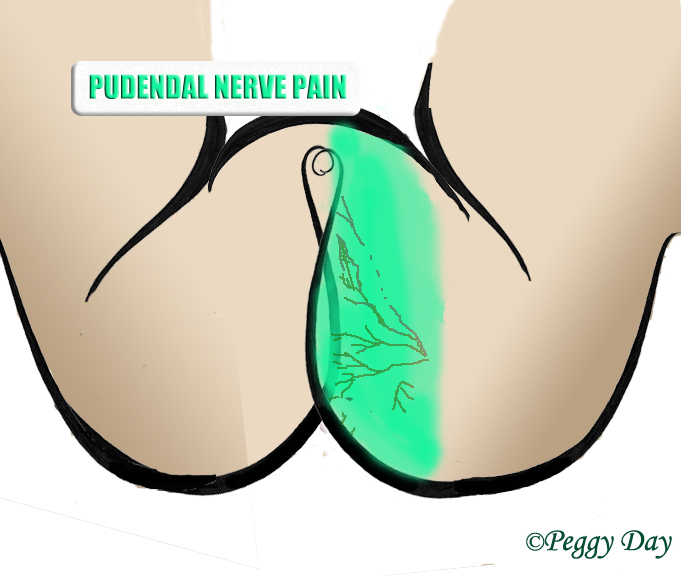
Patients with hypogastric entrapment really suffer from lumbar plexus entrapment syndrome with secondary affection of the sympathetic chain. The pain will be situated in the central pelvic floor, causing symptoms of prostatitis, vaginal, perineal or rectal pain that does not spread out to the periphery of the pelvic floor. It can affect the clitoris or glans of the penis. It tends to improve when sitting down (presuming there is no concurrent problem with the pudendal nerves, which, frankly, there often is), but immediately worsen when standing up (this stretches the lumbar plexus within the psoas major muscle). It will also worsen when walking uphill, running, or even flat-walking. A fluoroscopically guided nerve block to the inferior hypogastric plexus through the transsacral (S3 or S4 foramen) or para-coccygeal approaches may prove helpful in diagnosis, but is difficult to perform (Choi 2012). Much easier it is, to achieve worsening through strengthening of the psoas major muscle. This confirms the diagnosis.
Electrodiagnostic studies (Edx) are almost always normal. A normal test does not mean that the nerves are normal; disregard this completely. As with most entrapment problems, a proper clinical workup by an experienced physician is the best way to get diagnosed. EDx is helpful, however, in the diagnosis of autoimmune causes of neuropathies. MR neurographies rarely reveal thickening of the nerves or frank plexopathy. MRI is more helpful in excluding other causes, such as tumors that are compressing the plexuses or similar.
Treatment
Entrapment neuropathies do not tend to respond well to pharmacological treatment, and therefore it is helpful to initiate conservative treatment early on. Neurontin, Cymbalta, or Lyrica may help for some patients, but generally carry sideffects. More often than not, the drugs do not give significant relief of symptoms for these conditions. Opioids do not tend to be effective for neuropathic types of pain.
As already mentioned, the treatment for these conditions is very careful strengthening of the psoas major and piriformis and obturator internus muscles. This should be done twice per week, just one working set until mild fatigue. Mild worsening the subsequent day suggests correct execution, confirms the diagnosis, and also suggests that an appropriate volume of training was done. Anything more than “mild worsening” for one day, suggests too much work being done. For many of these patients, that can mean that they did 5 instead of 3 reps. The tolerance is often very poor, which also explains why they developed this problem in the first place. Treatment time can range between six months to 2 years depending on severity. Stretching weak muscles make them worse and must not be done. Thus, stretches for the deep hip rotators and hip flexors must not be done, as it makes the patient worse over time.
It is also important to avoid sitting on hard surfaces, and avoid sitting leaning forward or squatting for prolonged periods of time. Stretches for the pectineus and adductor brevis and adductor longus muscles can be helpful in increasing the capacity for forward-leaning.
The patient must evaluate themselves for stress and bracing. Having a chronic tendency to tensing up the abdomen, butt, or entire body, is common, and extremely detrimental. Work on relaxing. Gradually, it is possible to stop this pathological behavior.
References
- Spinosa JP, de Bisschop E, Laurencon J, Kuhn G, Dubuisson JB, Riederer BM. [Sacral staged reflexes to localize the pudendal compression: an anatomical validation of the concept]. Rev Med Suisse 2006;2(84):2416-8, 20-1
- Rousseff R, Tzvetanov P, Valkov I. Utility (or futility?) of electrodiagnosis in thoracic outlet syndrome. Electromyogr Clin Neurophysiol. 2005 Apr-May;45(3):131-3. PMID: 15981682.
- Larsen K, Chien GCC. Lumbosacral plexus entrapment syndrome. Part one: A common yet little-known cause of chronic pelvic and lower extremity pain. Anaesth pain & intensiv care 2019;23(2):124-137
- Choi HS, Kim YH, Han JW, Moon DE. A new technique for inferior hypogastric plexus block: a coccygeal transverse approach -a case report-. Korean J Pain. 2012;25(1):38-42. doi:10.3344/kjp.2012.25.1.38

Such a good article, you saved many people with your videos and articles and I’m gratfeul for this unexpected help. I have a question, maybe you have time to respond.
I saw one of your facebook posts and you said that non-traumatic lumbosacral plexus affection can cause extremity responses similar to CRPS. I have symptoms similar to CRPS (visible veins on penis, extensive enlarged veins expanding in pelvis seen by a MRI, hyperestesia, etc), but one thing makes me wonder if this is plausible. I don’t have pain, but I know for a fact that there were described painless cases of CRPS in literature. I also have premature ejaculation, sometimes ED and stuck nocturnal erection (maybe signs of sympatetic chain co-affection?)
What do you, it’s plausible that LPES is the cause for all those symptoms?
Refractory noctural erection (priapism) is possible in LPES, I have seen this before. But I have found ED and premature ejeculation to be vascular problem more so than a neurological problem, in most circumstances. You definitely don’t have CRPS.
Hi Kjetil. Thank you for the article. Is strengthening of the obturator internus muscles done with the clamshell exercise?
Can’t seem to find an exercise specifically for these muscles. Apologies, if I have overlooked something.
Best,
Anders
Piriformis exercise (45-80 degrees hip flexion, horizontal abduction) will get the obturator internus as well
Hi Kjetil, trank you so much vor this Artikel. I already did to many of your Piriformis exercise and got heaviest pain. I take it as proof. I‘ll try to find the right amount. Do you have a Suggestion on how to perform the pectineus strech you memtioned above?
Trank you so much.
Michaela
Kjetil, your articles have been incredibly helpful to me. For the last year I have been struggling through an unexpectedly difficult recovery following an inguinal hernia repair.
To make a very long story short it seems the insult from the hernia and/or the surgery detonated an occult time bomb of pelvic and lumbosacral dysfunction.
Fixing my posture re pelvic tilt (correcting my swayback stance) resulted in immediate improvement and a remarkable reduction in painful episodes. Now I am working on strengthening the psoas and piriformis as per this article.
Here is my question: when performing the leg lift for the psoas exercise, I feel resistance and then a firm snap in my hip. Is this normal/acceptable? Is this the “dancer’s hip” that says is either benign or debilitating depending on the article?
Thanks again for the effort you have put into the site, and congrats on med school!
Penultimate sentence should read: “ Is this the “dancer’s hip” that Google says is either benign or debilitating depending on the article?”
I have had pain off and on for over 15 years in my Lt hip/leg and into the perineum, rectum and urethra. Finding this article has been a true blessing. I had an unsuccessful pudendal nerve block and so far all PT has not been able to help regain remission.
My question is, have you seen patients that have had pain for 2 years, then go into a remission with no pain, just to reoccur again multiple times over time? Could there be a different impingement occurring causing this other than weak psoas, piriformis,etc?
I appreciate the reasearch so much after spending so many years with no understanding from doctors!
The patient will not just go into remission as such. They will gradually improve with diligence and persistence to the protocol. I have seen numerous patients fully recover.
Hi,
No, the snapping – presuming it is an iliopsoas “snap” – suggests that the psoas is not being engaged properly.
Thanks
Thank you so much for this info. I’m a super stressed person and have been having pudendal neuralgia for quite some time. I notice the pain with these exercises is only on my left side. Should I still do them on my right as well? I only did them 5 times and am already very sore. Would doing less make sense as it’s so little? Again thank you for this info!
Hi, yes. Train carefully and monitor your symptoms to avoid gross exacerbation.
Hello,
first, thanks for the great article, very informative. I’d like to ask you a question about my chronic symptoms, maybe you can help:
– Jelquing Injury Penis
– Happened 3 years ago
– Symptoms: Chronic flaccid penis pain. Unilateral, small spot, close to base. Not very strong, but long lasting discomfort / Pain
– Can not tell what really helps. Sometimes its gone, usually returns.
– No other symptoms apart from tingling down the foot sometimes
Now my question do you think this can be Pudendal Neuralgia?
Also i like to know if it is really advised to strenghten Hip Flexors and Piriformis for a person that sits all day ( me ) ?
Sorry for so many questions. Would appreciate it so much if you reply. I am grateful for any help. Thanks.
Can be, but I can’t know for sure without examination / QnA.
Kjetil, what are your thoughts on both strengthening and stretching affected muscles during treatment? Why would stretching harm the muscles if you are properly stimulating them with these exercises as well?
Thank you for the time you put into these fantastic articles and your videos.
Because weak muscles get worse by stretching
Had a conus medullaris spinal stroke. Left with unrelenting pudental neuralgia among other problems. Almost everything makes it worse except bring quiet and lying on my sides.
Any suggestions?
I have widespread nerve pain as you described in the article, i.e. Larsen & Chieng 2019 image+. I’m being tested for pectineus tendinitis/tear. Could this cause pudendal/sciatic nerve compression and burning pain as well as a significant limp with ambulating? Thank you.
Hi there, I note that this piriformis exercise is one that you consider superior to the ‘clamshell’ exercise due to the fact that the muscle is actually an abductor. I’m wondering whether we can include the so called ‘Fire-hydrant’ exercise in this group. The reason I ask is because I do struggle with this exercise but I love the logic behind it. Many thanks
Or just do what I recommend
I absolutely love your articles and videos. I’m so glad I found this site. Thank you so very much!
Thank you for this article! I have been suffering from Pudendal Neuralgia and what I think is inferior hypogastric plexalgia (zaps in the rectum which are mostly gone but flare up when I’m sitting for a long time or lying on a hard surface on my back). I have been going to PT for the pudendal neuralgia and found that my piriformis is very knotted up and tight. She will get me to about 95% and I will feel better, continue to do the exercises that she has prescribed but I cannot get back to 100%. I also notice I feel much better after she has worked on the piriformis. I am going to do the exercises you have listed in this article and I am going to focus on not tensing up so much. I am a runner and I also suffer from anxiety. I notice the flare up much more when I’m stressed. Thank you for this information, it’s really helpful. I wish I could visit your practice in person!
-Melanie
Kjetil,
Important Q: I suffer from SEVERE pudendal neuralgia, rectal nerve pain, hypogastric pain, psoas tightening and this explains my problem – Q: Why are you saying that worsening via strengthening the obturator, piriformis, and psoas major confirms the diagnosis yet, are also saying that the cure is to strengthen these muscles? Please help me understand this.
Because the way to resolve muscular dysfunction, at least in this scenario, is to train it, which causes mild inflammation, recovery, slight increase in work capacity, and then repeat the process until the dysfunction has been resolved. This can take months to years. During the inflammatory process, symptoms will worsen. The therapeutic window here is very narrow, and it is hard to do this properly.
Hi!
I’m having a lot of pain in what I believe is my pudendal nerve. I have been walking 3 times a day for the last 6 months, and the pain is getting worse. In the beginning is was a reliefe after sitting a whole day, but now the pain has gotten worse after a walk. What would you recomend for excercise with trubble with the PN?
The information is in the article