Myalgic encephalomyelitis (ME) is one of medicine’s grand mysteries. Its etiology is not known, and patients afflicted are rarely documented to recover from their ailment. Its diffuse presentation includes many symptoms, which implies that ME is actually an “umbrella diagnosis” for several underlying problems.
One of the problems with the ME diagnosis is that its symptoms are often compatible with those of migraines, fibromyalgia, and intracranial hypertension. Global “tenderness” (diffuse and idiopathic myofascial pain), frequent headaches with or without visual impairment, severe fatigue, orthostatic dysfunction (such as postural orthostatic tachycardia syndrome (POTS)), cognitive impairment which especially may affect memory, dysarthria, frequent illness, and more (Carruthers 2003, 2011; Fukuda 1994; Jason 2010; NICE, 2007). Could it be that several underlying problems are clustering into ME?
Although this is a short article, the aim here is to demonstrate the potential of biomechanical factors which may derange cerebral function.
NB: THIS ARTICLE IS FOR EDUCATIONAL PURPOSES ONLY
A logical mechanism and potential cause of ME?
Having examined many patients with ME, my impression is that they are actually suffering from multiple problems whose symptoms are generally diffuse and hard to pinpoint. For example, I have not seen one patient with ME who did not test positive for thoracic outlet syndrome (TOS) using Selmonosky’s diagnostic triad (Selmonosky 1982, 2002, 2008). Further, many ME patients have proven venous obstruction, especially at the atlantostyloid interval (Higgins 2015), and are reported to have high intracranial pressures (Higgins 2017, Hulens 2018). Higgins (2017) claim that the symptoms in patients with idiopathic intracranial hypertension are largely compatible to those of ME, and they postulate that ME, in reality, may be an early symptom of raised intracranial pressures (ICP). It is well known that increased ICP is associated with fatigue. There is also a high prevalence of anxiety and depression in ME patients (Daniels 2017), and as I’ve written about before, patients with anxiety tend to brace themselves (Article: Involuntary muscle clenchers), which also increases ICP, exacerbating the underlying problem.
As I’ve written about before, and I am also currently working on a scientific paper on the topic, TOS may cause cerebral hyperperfusion (Larsen 2018c; Article: Vertigo). Distal subclavian artery compression, also in the absence of conspicuous brachial ischemia (“arterial TOS”), will cause the blood that is prevented from entering the brachium to redirect and be forced into the nearest vessels, i.e. the vertebral and carotid arteries which supply the brain. It is known that patients with ME have cold hands (Nacul 2011b) and low blood pressures [especially during ambulation] (Newton 2009), which is exactly what happens when there is distal subclavian compression. This may saturate the arterial system and contribute to intracranial hypertension (ICH). As the subclavian artery compresses due to TOS, the brachial plexus may as well, potentially causing diffuse pains in the chest, upper back, and arms, in addition to [the potential presence of] fatigue, visual impairment, migraines, and dizziness. It is my experience that “vertebrocarotid hyperperfusion” is an occult but common sequela of TOS, explaining its common presence in patients with seemingly cephalogenic problems. Longstanding ICH may frequently cause spontaneous cerebrospinal fluid leaks (Osborn’s brain 2nd ed., 2017), offering an explanation as to why many of these patients develop sudden orthostatic incompetence.
We suggest, therefore, that incomplete forms of idiopathic intracranial hypertension are not subclinical and irrelevant but clinically important and numerically significant, and may manifest as chronic fatigue syndrome. Unknown, of course, is what proportion of patients with chronic fatigue syndrome might represent a variant of IIH but it could be substantial [12], [13]. In which case IIH and an unknown but potentially significant number of cases of chronic fatigue syndrome could be considered as different expressions of the same disorder of intracranial pressure, essentially part of a spectrum in which IIH in full would represent the least common and most extreme disturbance while incomplete forms, including IIH without papilledema and chronic fatigue syndrome, represent the less severe but more common. – Higgins et al., 2017
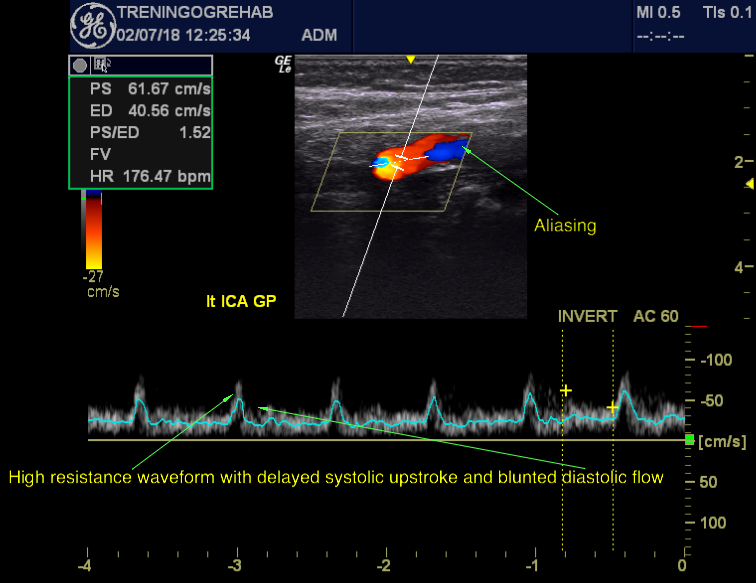
Fig. 1: Ultrasound showing pyramidic systolic peaks with decreased diastolic flow due to cerebrovascular saturation and venous congestion in patient with TOS and ME. He also has bilateral IJV obstruction. Severe carotid rigidity and fullness were noted upon palpation, although the patient was only 25 years old. The heart rate is falsened by the dicrotic notch.
Many of these patients have very poor cervical and thoracic postures. This is a known finding in TOS patients (Telford 1948, Swift 1984, Selmonosky 2002, Larsen 2018b) as well. Poor postures may stability impairment of the upper cervical spine, contributing to facet joint misalignments (Goel 2011; 2015; Riascos 2015; Larsen 2018c). Now, facet joint subluxation at the atlanto-occipital junction, a controversial but real problem, may cause compression of the internal jugular veins (IJV) (Larsen 2018c). Compression at this interval has been noted by many authors (Seoane 1999, Gweon 2011, Dashti 2012, Jayaraman 2012, Higgins 2015). Seoane (1999) also noted that the IJV compression may be positional, e.g. increasing with rotation or extension of the neck. I noted the same, in my 2018 study linked above. Now, if a patient has both TOS and blocked IJVs, this would involve various degrees of arterial hyperperfusion simultaneous with impaired venous drainage – a very unfortunate tandem that is likely to cause significant ICH.
If there is bilateral [internal jugular] venous obstruction or obstruction of the dominant sinus, cerebral hypoperfusion may occur, as not enough fresh blood is able to enter the head due to saturation (Ferro 2003, Masuhr 2006). In very serious circumstances (usually in cerebral thrombosis), brain ischemia with infarct may take place. Generally, however, e.g. with biomechanical venous obstruction, there will be borderline cerebral hypoxia which causes [severe] fatigue, memory loss, dizziness, depression, lethargy, nausea, migraines, visual impairment, etc. (Higgins 2015)
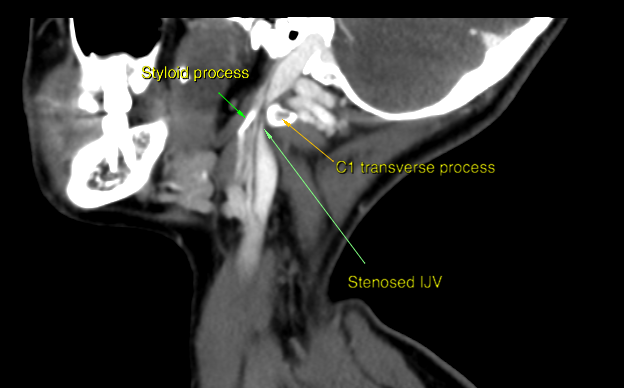
Fig. 2: Patient with chronic migraines and ME. Bilateral C1 subluxation and IJV obstruction
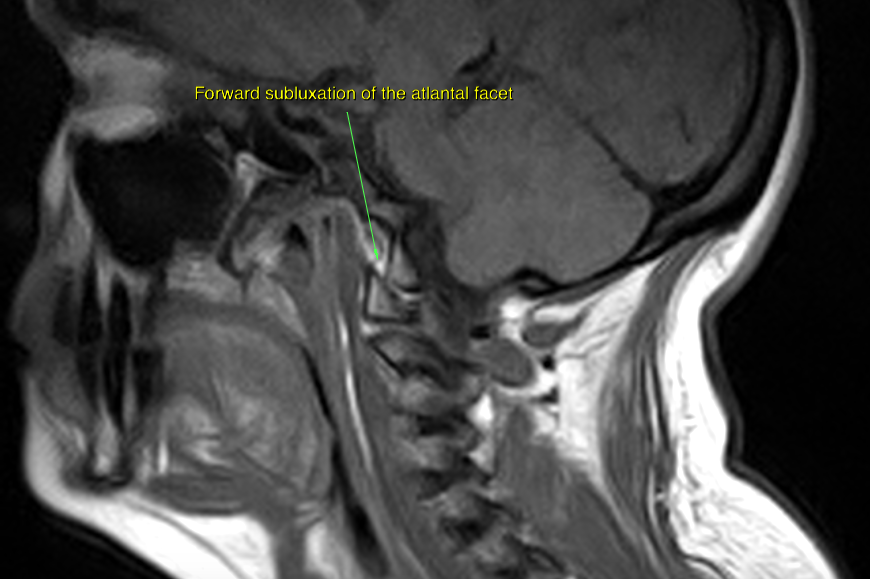
Fig. 3: Significant atlanto-occipital facet subluxation in another patient
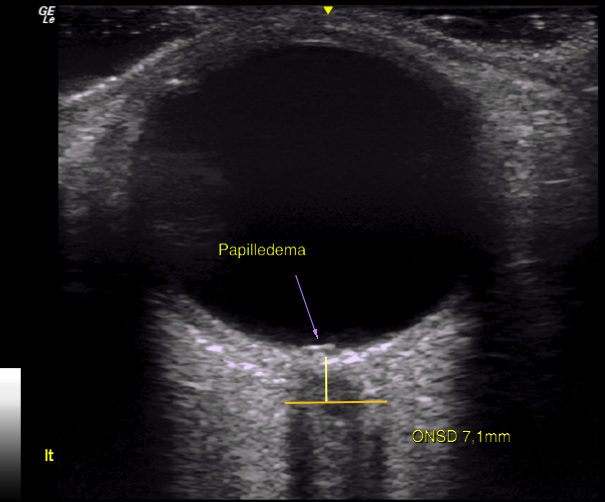
Many patients will not have abnormal lumbar puncture opening pressures (Higgins 2015, 2019; Larsen 2018b; Mokri 1997; Schievink 2011, Suh & Kim 2013, Higgins 2013, Clark 1994, Abdelfatah 2017), possibly due to compensatory CSF leakage (Osborn’s brain 2nd ed. 2017, Higgins 2015). Unilateral IJV blockage may also be symptomatic, especially if the dominant transverse sinus is obstructed (Cumurciuc 2005; Hyun-Ah Kim 2008; Karaman 2009, Thandra 2015; Zhou 2018), or if there is co-presence of TOS. The best diagnostic criteria for increased ICP is dilation of the optic nerve sheaths, which seems to be present even if the patient has a suspected leak or normal pressures upon lumbar puncture. A systematic review and meta-analysis (Geeraerts 2008) states that optic nerve sheath diameter (ONSD) above 5,7 mm highly suggests aberrant ICP. ONSD is not always well visualized on MRI due to high slice thicknesses, but may easily be detected with ultrasound (or MRI with narrower slice thickness)
Fig. 4: Patient with TOS, chronic fatigue syndrome as well as light sensitivity (no migraines nor headaches), with severely distended optic nerve sheaths.
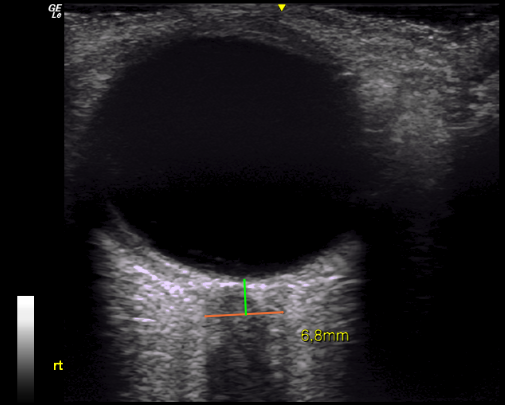
Fig. 5: Right eye of the same patient.
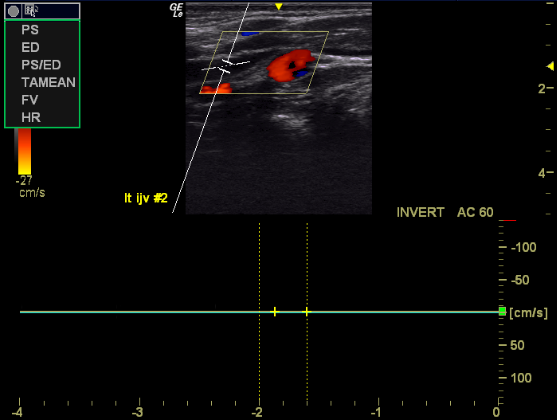
Fig. 5: Also the same patient. An absence of flow in the left IJV. Right IJV had excess [compensatory] flow of 600ml/min.
Longstanding poor cervical postures will also negatively impact the cervical muscles, resulting in nerve entrapment neuropathies, sometimes affecting the autonomic nervous system. Thoracic outlet syndrome, for one, involves entrapment of the brachial plexus. The brachial plexus has autonomic components to it, but it also directly anastomoses with the sympathetic chain. Further, the vagus nerve traverses between the scalenus anticus and sternocleidomastoid muscles. There are several reports of TOS causing dysfunction of the autonomic system (Urschel 2007, 2010; Aralasmak 2010, Yamagami 1994, Shreeve 2011, Sanders 2007). Moreover, between the longus capitis and alar fascia of the upper neck traverses the cervical sympathetic chain (Civelek et al., 2008), and its ganglia also reside there.
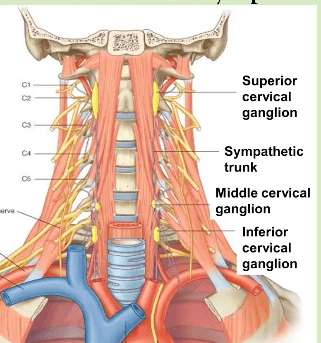
Severe weakness of the longus capitis, again due to poor posture, may cause entrapment of these nerves and result in dysfunction. The cervical ganglia innervates the carotid and vertebral arteries, and also directly anastomosis with the glossopharyngeal nerve which innervates the carotid sinus (Porzionato 2019), the latter a key component of cerebral autoregulation. Irritation of the sympathetic chain may induce cerebral vasoconstriction and thus raises blood pressure (Tameem 2013). This will greatly exacerbate cerebrovascular hypertension in the co-presence of TOS. Further, the superior cervical ganglion, its dysfunction that is, has been implicated in tinnitus, visual and vestibular disorders, such as Meniere’s disease (Franz 1998, McDougal 2015, Garnett Passe “Sympathectomy in Relation to Meniere’s Disease, Nerve Deafness and Tinnitus“). Tremendous weakness of these muscles are common in ME patients, and reproduction & exacerbation of symptoms generally occur upon strengthening, confirming their association. For instance, I have seen strengthening exercises for the longus capitis severely affect POTS patients, exacerbating upright tachycardia even when using antagonistic medicine (thus ME patients must be extremely careful when initiating these corrective exercises). I postulate that entrapment of these nerves may derange the cerebrovascular autoregulative system.
What about the many reports of immune system impairment in these patients? I think it is misunderstood. A chronic state of fatigue will also cause immune weakness in generally healthy individuals. For example, it is known that athletes who overtrain also develop immune system weakness (Hackney 2012, 2015; Teixeira Guimarães 2017). It is also known that general overworking, stress etc. will negatively affect the immune system. Thus I postulate that the immune reactions seen in ME patients may not be ME specific symptoms, but typical symptoms of living in a state of chronic exhaustion.
Barometrically influenced
A common report from patients with ME is that their condition improves when they visit warmer countries or in higher barometric pressures (Bested & Marshall, 2015), meaning that they worsen when it’s cold and rainy. Many migraine patients report the same (Hoffman 2011; 2015), as do fibromyalgia patients (Bossema 2013), and those afflicted with vertigo (Saeed & Omari, 2016).
Although not all ME patients have migraines (it must be stated that clinically, raised ICP and migraines are indistinguishable! – Mathew 1996, Wang 1998, Vieira 2008, Sina 2017), there is some evidence which may help in explaining this phenomenon. As I’ve written about before (in my migraine article), I strongly consider migraines to be vasculogenic, mainly caused by cerebrovascular congestion (CVC). CVC involves forced dilation of the parenchymal vessels, activating the trigeminovascular response which is thought to trigger the attacks (Gooriah 2015). When the weather changes for the worse, barometric pressures reduce, and this may induce peripheral vasoconstriction (Sato 2003) and cerebral vasodilation (Okuma 2015). Peripheral resistance causes more blood to be forced into the already congested cerebrovascular system, increasing ICP and triggering/worsening migraines. This gentle increase in ICP is too small to affect a healthy individual; the reason it affects ME patients is, in my impression, because they were already on the edge of the knife, and is thus, functionally, the “last drop”.
This cerebrovascular effect induced by barometric alterations, seen in the light of what I propose in this article, may explain why so many ME patients prefer warmer climates.
The pain course of subjects suffering from migraine is influenced by weather conditions (14, 15). Possible mechanisms underlying such relationship have been investigated in animal models, where changes in atmospheric pressure and temperature were found to be linked to peripheral vasoconstriction, a local increase in algesic substances and adrenaline with a general decrease in central and peripheral sensory pain thresholds (16). … It was found that a low-pressure environment worsens pain by promoting the sympathetic activity, which in turn causes local vasoconstriction and ischaemia (25). Low-temperature increases pain through still unclear mechanisms, which include an increase in blood pressure, heart rate and noradrenaline levels (16). A cold environment may also favour the release of peripheral mediators, thus inducing vasoconstriction, local ischaemia and promoting the release of algesic substances by non-neuronal cells (16). – Cioffi et al., 2017
Barometric pressure change can be one of the exacerbating factors of migraine headaches. – Kimoto et al., 2011
The onset of an attack as well as high headache intensity was associated with lower temperature and higher humidity. Our data indicate that a subgroup of migraineurs is highly sensitive to changes of certain weather components – Hoffmann et al., 2011
Small decreases of 6–10 hPa relative to the standard atmospheric pressure of 1013 hPa induced migraine attacks most frequently in patients with migraine. … This is consistent with the idea that small atmospheric changes trigger migraine via the following mechanism (Welch et al. 1993; Lauritzen 1994; Lance et al. 1983; Silberstein and Silberstein 1990): (1) first, a small decrease in barometric pressure causes dilatation of cerebral blood vessels, leading to serotonin release from platelets, (2) increased levels of blood serotonin induce vasoconstriction and the onset of aura, and (3) finally, the subsequent decrease of serotonin causes rapid dilatation of cerebral blood vessels, thereby triggering migraine. This is consistent with the common observation that the temporary decrease in cerebral blood flow during CSD is caused by constriction of both the superficial and parenchymal blood vessels, whereas the post-CSD rise in cerebral blood flow is primarily related to the dilatation of parenchymal blood vessels. – Okuma et al., 2015
The most common trigger factors experienced by the patients were weather (82.5%), stress (66.7%), menstruation (51.4%) and relaxation after stress (50%). – Wöber et al., 2006
The highest frequencies of weather-related symptoms were reported in … Germany were headache/migraine (61%), lethargy (47%), sleep disturbances (46%), fatigue (42%), joint pain (40%), irritation (31%), depression (27%), vertigo (26%), concentration problems (26%) and scar pain (23%). … In Germany 32% of the weather-sensitive subjects reported themselves to be unable to do their regular work because of weather-related symptoms at least once in the previous year, and 22% of them several times. – Mackensen et al., 2005
Psychological factors
As stated, ME has been associated with stress and anxiety (Daniels 2017). What is the mechanism of impairment? A common tendency of people who are very stressed, scared, anxious etc., is that they hold their breaths and brace their bodies. I call this phenomenon “global involuntary clenching strategy” (GICS), where the patient is more or less constantly creating valsalva maneuver due to an inability to handle stress. Constant valsalva will cause increased intracranial pressures as well as muscle imbalances, and may therefore be directly linked to ME dysfunctions and not merely an amplifying factor.
This bracing strategy is very common. I frequently find it in TOS patients, especially patients with TOS who do not have a logical explanation (e.g. whiplash) for their condition. It is also present in most patients with lumbar plexus compression syndrome and vestibular disorders. I will not elaborate upon this topic here, but rather you can read about it in my GICS article.
In conclusion
It is my impression that myalgic encephalomyelitis is an umbrella diagnosis covering several subproblems. I have not seen a patient with “ME” who did not have thoracic outlet syndrome based on Selmonosky’s diagnostic triad criteria of diagnosis. TOS causes (one or more of the following) cerebrovascular hyperperfusion and thus congestion, arm, chest, neck and chest pain. It has also been implicated in dysautonomia. Its symptoms are often nonspecific and difficult to pinpoint, and its presentation may vary from patient to patient. The co-presence of internal jugular vein stenosis may greatly impair cerebral blood drainage, thus increasing congestion and intracranial pressures, worsening the situation. Longstanding intracranial hypertension may cause spontaneous CSF leaks and concomitant orthostatic incompetence.
Poor weather may add to this by causing peripheral vasodilation, mimicking the Cushing effect, as it forces more blood into the [already congested] head, making the patient worse. Stress and anxiety may cause the patient to “brace themselves”, once again further worsening muscle imbalances, posture, and intracranial pressure.
Treatment of ME must, therefore, be multifactorial. Stress and especially global bracing must be removed as soon as possible. A suggested approach is detailed in my GICS article, linked above. Further, posture must be optimized, especially paying attention to the thoracic outlet and the upper cervical spine, as problems here may directly affect cerebral blood flow and ICP, whose aberrancies I believe to be the main drivers of myalgic encephalomyelitis.
I have written about specific mechanisms and treatment of the neck, jaw, pelvis etc so many times. Please confer with my other articles with regards to specific diagnosis and treatment. The point of this article was to detail mechanisms which may lead to ME. There is not “one ME treatment”, but rather treatments for upper cervical dysfunction, thoracic outlet syndrome, raised ICP, etc., which in turn may ameliorate the ME symptoms.
Although complex, the good news is that most of these conditions are treatable, but please be very careful when initiating exercises for this condition, as patients with ME tend to have very poor tolerances. It takes time. Below I have provided free reading material which explains these mechanisms, diagnoses and treatment strategies quite thoroughly:
- https://treningogrehab.no/atlas-joint-instability-causes-consequences-solutions/
- https://treningogrehab.no/multifactorial-causes-solutions-chronic-neck-pain/
- https://treningogrehab.no/treating-migraine-headaches-addressing-atlas-thoracic-outlet/
- https://treningogrehab.no/how-truly-treat-thoracic-outlet-syndrome/
- https://treningogrehab.no/association-tinnitus-neck-tmj/
- https://treningogrehab.no/vestibular-impairment-and-its-association-to-the-neck-and-tmj/
- https://treningogrehab.no/true-cause-solution-temporomandibular-dysfunction-tmd/
- https://treningogrehab.no/identify-treat-lumbar-plexus-compression-syndrome-lpcs/
Attached are some videos which demonstrate proper posture, bracing, etc.
References
- Carruthers BM, Jain AK, De Meirleir KL, et al. Myalgic Encephalomyelitis/Chronic Fatigue Syndrome. J CFS Pages 7-115 | Received 12 Feb 2002, Accepted 17 May 2002, Published online: 04 Dec 2011
- Carruthers BM, van de Sande MI, de Meirleir KL, et al. Myalgic encephalomyelitis: International Consensus Criteria. J Intern Med 2011; 270: 327–338. https://doi.org/10.1111/j.1365-2796.2011.02428.x
- Fukuda K, Straus SE, Hickie I, Sharpe MC, Dobbins JG, Komaroff A. The chronic fatigue syndrome: a comprehensive approach to its definition and study. International Chronic Fatigue Syndrome Study Group. Ann Intern Med. 1994 Dec 15;121(12):953-9. doi: 10.7326/0003-4819-121-12-199412150-00009. PMID: 7978722.
- Jason LA, Evans M, Porter N, Brown M, Brown AA, Hunnell J, Friedberg F. The development of a revised Canadian myalgic encephalomyelitis chronic fatigue syndrome case definition. American Journal of Biochemistry and Biotechnology. 2010;6:120–135. doi: 10.3844/ajbbsp.2010.120.135.
- NICE GUIDANCE. Chronic fatigue syndrome/myalgic encephalomyelitis (or encephalopathy): diagnosis and management Clinical guideline [CG53]Published date: 22 August 2007
- Selmonosky CA, Byrd R, Blood C, Blanc JS. Useful triad for diagnosing the cause of chest pain. South Med J. 1981;74:974-949.
- Selmonosky CA, Poblete Silva R. The diagnosis of thoracic outlet syndrome. Myths and Facts. Chilean J of Surg. 2008;60(3):255-261.
- Selmonosky CA. The white hand sign. A new single maneuver useful in the diagnosis of thoracic outlet syndrome. Southern Med Journal. 2002;85:557.
- Higgins JNP, Pickard JD, Lever AML. Chronic fatigue syndrome and idiopathic intracranial hypertension: Different manifestations of the same disorder of intracranial pressure? Med Hypotheses. 2017 Aug;105:6-9. doi: 10.1016/j.mehy.2017.06.014. Epub 2017 Jun 24. PMID: 28735654.
- Hulens M, Rasschaert R, Vansant G, Stalmans I, Bruyninckx F, Dankaerts W. The link between idiopathic intracranial hypertension, fibromyalgia, and chronic fatigue syndrome: exploration of a shared pathophysiology. J Pain Res. 2018;11:3129-3140. Published 2018 Dec 10. doi:10.2147/JPR.S186878
- Daniels J, Brigden A, Kacorova A. Anxiety and depression in chronic fatigue syndrome/myalgic encephalomyelitis (CFS/ME): Examining the incidence of health anxiety in CFS/ME. Psychol Psychother. 2017 Sep;90(3):502-509. doi: 10.1111/papt.12118. Epub 2017 Feb 28. PMID: 28244209.
- Larsen K, Galluccio FC, Chand SK.Does thoracic outlet syndrome cause cerebrovascular hyperperfusion? Diagnostic markers for occult craniovascular congestion. Anaesth pain intensive care 2020;24(1)69-86. DOI: https://doi.org/10.35975/apic.v24i1.1230
- Larsen K. Occult intracranial hypertension as a sequela of biomechanical internal jugular vein stenosis: A case report. Anaesth Pain & Intensive Care 2018;22(2)
- Nacul LC, Lacerda EM, Pheby D, et al. Prevalence of myalgic encephalomyelitis/chronicfatigue syndrome (ME/CFS) in three regions of England: a repeated cross-sectional study inprimary care. BMC Medicine2011,9:91http://www.biomedcentral.com/1741-7015/9/91
- Newton JL, Sheth A, Shin J, et al. Lower Ambulatory Blood Pressure in Chronic Fatigue Syndrome. March 2009Psychosomatic Medicine 71(3):361-5 DOI: 10.1097/PSY.0b013e31819ccd2a
- Osborn AG, Hedlund G, Salzman KL.Osborn’s Brain. 2nd edition. Elsevier;2017.
- Telford ED, Mottershead S. Pressure of the cervicobrachial junction. J Bone Joint Surg Am. 1948;30:249.
- Swift TR, Nichols FT. The droopy shoulder syndrome. J Neurology 1984; 34, 212- 215.
- Goel A. Facet distraction-arthrodesis technique: Can it revolutionize spinal stabilization methods?. J Craniovertebr Junction Spine. 2011;2(1):1-2. doi:10.4103/0974-8237.85306
- Goel A. Vertical facetal instability: Is it the point of genesis of spinal spondylotic disease?. J Craniovertebr Junction Spine. 2015;6(2):47-48. doi:10.4103/0974-8237.156031
- Riascos R, Bonfante E, Claudia C, Guirguis M, Hakimelahi R, West C. Imaging of Atlanto-Occipital and Atlantoaxial Traumatic Injuries: What the Radiologist Needs to Know. RadioGraphics 2015; 35:2121–2134 DOI: 10.1148/rg.2015150035
- Seoane E, Rhoton AL Jr. Compression of the internal jugular vein by the transverse process of the atlas as the cause of cerebellar hemorrhage after supratentorial craniotomy. Surg Neurol. 1999 May;51(5):500-5. doi: 10.1016/s0090-3019(97)00476-x. PMID: 10321879.
- Gweon HM, Chung TS, Suh SH. Evaluation of the Cause of Internal Jugular Vein Obstruction on Head and Neck Contrast Enhanced 3D MR Angiography Using Contrast Enhanced Computed Tomography. JKSMRM 15:41-47(2011)
- Dashti SR, Nakaji P, Hu YC, Frei DF, Abla AA, Yao T, et al. Styloidogenic jugular venous compression syndrome: diagnosis and treatment: case report. Neurosurgery. 2012 Mar;70(3):E795-9. doi: 10.1227/NEU.0b013e3182333859
- Jayaraman MV, Boxerman JL, Davis LM, Haas RA, Rogg JM. Incidence of extrinsic compression of the internal jugular vein in unselected patients undergoing CT angiography. AJNR Am J Neuroradiol. 2012 Aug;33(7):1247-50. doi: 10.3174/ajnr.A2953. Epub 2012 Feb 9. PMID: 22322614.
- Ferro JM, Canhao P, Stam J, et al. Prognosis of Cerebral Vein and Dural Sinus Thrombosis. Stroke. 2004;35:664–670. https://doi.org/10.1161/01.STR.0000117571.76197.26
- Masuhr F, Busch M, Amberger N, Ortwein H, Weih M, Neumann K, Einhäupl K, Mehraein S. Risk and predictors of early epileptic seizures in acute cerebral venous and sinus thrombosis. Eur J Neurol. 2006 Aug;13(8):852-6. doi: 10.1111/j.1468-1331.2006.01371.x. PMID: 16879295.
- Higgins N, Trivedi R, Greenwood R, Pickard J. Brain slump caused by jugular venous stenoses treated by stenting: a hypothesis to link spontaneous intracranial hypotension with idiopathic intracranial hypertension. J Neurol Surg Rep. 2015 Jul;76(1):e188–e193. doi: 10.1055/s-0035-1555015
- Higgins JN et al. Headache, cerebrospinal fluid leaks, and pseudomeningoceles after resection of vestibular schwannomas: efficacy of venous sinus stenting suggests cranial venous outflow compromise as a unifying pathophysiological mechanism. J Neurol Surg B. DOI: 10.1055/s-0039-1677706
- Mokri B, Hunter SF, Atkinson JLD, Piepgras DG: Orthostatic headaches caused by CSF leak but with normal CSF pressures. Neurology 1998, 51:786–790.
- Schievink WI, Dodick DW, Mokri B, et al. Diagnostic criteria for headache due to spontaneous intracranial hypotension: a perspective. Headache. 2011;51(9):1442–1444. doi: 10.1111/j.1526-4610.2011.01911.x.
- Suh SY, Kim SJ. IIH with normal CSF pressures? Indian J Ophthalmol. 2013 Nov;61(11):681-2. doi: 10.4103/0301-4738.119416. PMID: 24145570; PMCID: PMC3959092.
- Higgins N, Pickard J, Lever A. Lumbar puncture, chronic fatigue syndrome and idiopathic intracranial hypertension: a cross-sectional study. JRSM Short Rep. 2013 Nov 21;4(12):2042533313507920. doi: 10.1177/2042533313507920. PMID: 24475346; PMCID: PMC3899735.
- Clark D, Bullock P, Hui T, Firth J. Benign intracranial hypertension: a cause of CSF rhinorrhoea. J Neurol Neurosurg Psychiatry. 1994 Jul;57(7):847-9. doi: 10.1136/jnnp.57.7.847. PMID: 8021676; PMCID: PMC1073032.
- Abdelfatah MA. Normal Pressure Pseudotumor Cerebri: A Series of Six Patients. Turk Neurosurg. 2017;27(2):208-211. doi: 10.5137/1019-5149.JTN.15846-15.1. PMID: 27593779.
- Cumurciuc R, Crassard I, Sarov M, Valade D, Bousser MG. Headache as the only neurological sign of cerebral venous thrombosis: a series of 17 cases. J Neurol Neurosurg Psychiatry. 2005 Aug;76(8):1084-7. doi: 10.1136/jnnp.2004.056275. PMID: 16024884; PMCID: PMC1739763.
- Kim HA, Sohn SI, Lee H. Cerebral venous thrombosis mimicking acute unilateral vestibulopathy. Neurol Sci. 2008 Feb;29(1):41-3. doi: 10.1007/s10072-008-0858-9. Epub 2008 Apr 1. PMID: 18379740.
- Karaman E, Saritzali G, Cansiz H. A case of increased intracranial pressure after unilateral modified radical neck dissection. Am J Otolaryngol. 2009 Jul-Aug;30(4):261-3. doi: 10.1016/j.amjoto.2008.04.007. Epub 2008 Sep 21. PMID: 19563938.
- Thandra A, Jun B, Chuquilin M. Papilloedema and Increased Intracranial Pressure as a Result of Unilateral Jugular Vein Thrombosis. Neuroophthalmology. 2015 Jul 15;39(4):179-182. doi: 10.3109/01658107.2015.1044541. PMID: 27928352; PMCID: PMC5123161.
- Zhou D, Meng R, Zhang X, Guo L, Li S, Wu W, Duan J, Song H, Ding Y, Ji X. Intracranial hypertension induced by internal jugular vein stenosis can be resolved by stenting. Eur J Neurol. 2018 Feb;25(2):365-e13. doi: 10.1111/ene.13512. Epub 2017 Dec 7. PMID: 29114973.
- Geeraerts T, Newcombe VF, Coles JP, Abate MG, Perkes IE, Hutchinson PJ, Outtrim JG, Chatfield DA, Menon DK. Use of T2-weighted magnetic resonance imaging of the optic nerve sheath to detect raised intracranial pressure. Crit Care. 2008;12(5):R114. doi: 10.1186/cc7006. Epub 2008 Sep 11. PMID: 18786243; PMCID: PMC2592740.
- Aralasmak A, Karaali K, Cevikol C, Uysal H, Senol U. Open Access MR Imaging Findings in Brachial Plexopathy with Thoracic Outlet Syndrome. American Journal of Neuroradiology March 2010, 31 (3) 410-417; DOI: https://doi.org/10.3174/ajnr.A1700
- Urschel HC, Kourlis H. Thoracic outlet syndrome: a 50-year experience at Baylor University Medical Center. Proc (Bayl Univ Med Cent). 2007 Apr;20(2):125-35. doi: 10.1080/08998280.2007.11928267. PMID: 17431445; PMCID: PMC1849872.
- Yamagami T, Handa H, Higashi K, Kaji R. Brachial plexus injury with cough attack: case report. Neurosurgery. 1994 Jun;34(6):1084-6; discussion 1086. doi: 10.1227/00006123-199406000-00023. PMID: 8084397.
- Kaymak B, Ozçakar L, Oğuz AK, Arsava M, Ozdöl C. A novel finding in thoracic outlet syndrome: tachycardia. Joint Bone Spine. 2004 Sep;71(5):430-2. doi: 10.1016/j.jbspin.2003.07.007. PMID: 15474397.
- Shreeve MW, La Rose JR. Chiropractic care of a patient with thoracic outlet syndrome and arrhythmia. J Chiropr Med. 2011;10(2):130-134. doi:10.1016/j.jcm.2010.09.002
- Civelek E, Karasu A, Cansever T, Hepgul K, Kiris T, Sabanci A, Canbolat A. Surgical anatomy of the cervical sympathetic trunk during anterolateral approach to cervical spine. Eur Spine J. 2008 Aug;17(8):991-5. doi: 10.1007/s00586-008-0696-8. Epub 2008 Jun 12. PMID: 18548289; PMCID: PMC2518767.
- Porzionato A, Macchi V, Stecco C, De Caro R. The Carotid Sinus Nerve-Structure, Function, and Clinical Implications. Anat Rec (Hoboken). 2019 Apr;302(4):575-587. doi: 10.1002/ar.23829. Epub 2018 May 2. PMID: 29663677.
- Tameem A. Cerebral physiology. Continuing Education in Anaesthesia Critical Care & Pain, Volume 13, Issue 4, August 2013, Pages 113–118, https://doi.org/10.1093/bjaceaccp/mkt001
- Hackney AC, Koltun KJ. The immune system and overtraining in athletes: clinical implications. Acta Clin Croat. 2012 Dec;51(4):633-41. PMID: 23540172.
- Hackney AC, Lane AR. Exercise and the Regulation of Endocrine Hormones. Prog Mol Biol Transl Sci. 2015;135:293-311. doi: 10.1016/bs.pmbts.2015.07.001. Epub 2015 Aug 5. PMID: 26477919.
- Guimarães TT, Terra R, Dutra PML. Chronic effects of exhausting exercise and overtraining on the immune response: Th1 and Th2 profile. Motricidade 2017, vol. 13, n. 3, pp. 69-78
- Bested AC, Marshall L. Review of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: An evidence-based approach to diagnosis and management by clinician. November 2015Reviews on Environmental Health 30(4):223-249 DOI: 10.1515/reveh-2015-0026
- Hoffmann J, Lo H, Neeb L, et al. Weather sensitivity in migraineurs. J Neurol. 2011;258:596–602.
- Hoffmann J, Schirra T, Lo H, Neeb L, Reuter U, Martus P. The influence of weather on migraine – are migraine attacks predictable?. Ann Clin Transl Neurol. 2015;2(1):22-28. doi:10.1002/acn3.139
- Bossema ER, van Middendorp H, Jacobs JW, Bijlsma JW, Geenen R. Influence of weather on daily symptoms of pain and fatigue in female patients with fibromyalgia: a multilevel regression analysis. Arthritis Care Res (Hoboken). 2013 Jul;65(7):1019-25. doi: 10.1002/acr.22008. PMID: 23737338.
- Saeed BMN, Omari AF. Climatic variations and benign paroxysmal positional vertigo. J Otol. 2016 Mar;11(1):33-37. doi: 10.1016/j.joto.2016.03.002. Epub 2016 Mar 19. PMID: 29937808; PMCID: PMC6002593.
- Mathew NT, Ravishankar K, Sanin LC. Coexistence of migraine and idiopathic intracranial hypertension without papilledema. Neurology. 1996 May;46(5):1226-30. doi: 10.1212/wnl.46.5.1226. PMID: 8628457.
- Wang SJ, Silberstein SD, Patterson S, Young WB. Idiopathic intracranial hypertension without papilledema: a case-control study in a headache center. Neurology. 1998 Jul;51(1):245-9. doi: 10.1212/wnl.51.1.245. PMID: 9674810.
- Vieira DS, Masruha MR, Gonçalves AL, Zukerman E, Senne Soares CA, Naffah-Mazzacoratti Mda G, Peres MF. Idiopathic intracranial hypertension with and without papilloedema in a consecutive series of patients with chronic migraine. Cephalalgia. 2008 Jun;28(6):609-13. doi: 10.1111/j.1468-2982.2008.01564.x. Epub 2008 Mar 31. PMID: 18384415.
- Sina F, Razmeh S, Habibzadeh N, Zavari A, Nabovvati M. Migraine headache in patients with idiopathic intracranial hypertension. Neurol Int. 2017 Oct 2;9(3):7280. doi: 10.4081/or.2017.7280. PMID: 29071043; PMCID: PMC5641834.
- Gooriah R, Nimeri R, Ahmed F. Evidence-Based Treatments for Adults with Migraine. Pain Res Treat. 2015;2015:629382. doi: 10.1155/2015/629382. Epub 2015 Dec 29. PMID: 26839703; PMCID: PMC4709728.
- Sato J. Weather change and pain: A behavioral animal study of the influences of simulated meteorological changes on chronic pain. April 2003International Journal of Biometeorology 47(2):55-61 Follow journal DOI: 10.1007/s00484-002-0156-9
- Okuma H, Okuma Y, Kitagawa Y. Examination of fluctuations in atmospheric pressure related to migraine. Springerplus. 2015;4:790. Published 2015 Dec 18. doi:10.1186/s40064-015-1592-4



This article has clearly defined – me! I am at least 20 years experienced in this painful labyrinth, and the self-study. You seem to be quite accurate! But I remain desperate for help.
Hello,
my name is Pedja Zivanovic and I am a doctor, physiatrist from Serbia. I think that yout articles are great- finally an explanation for those strange symptoms of cervical origin. I would like to use the opportunity to ask you if you have some advice about hiatal hernia, which can also be a reason for a lot of unpleasant symptoms.
Yours gratefuly, dr Pedja Zivanovic
Hello doc and thanks. The most common “habitual” cause of hiatal hernia is stress and breath holding. I have seen patients recover without surgery with diaphragm massages and respiratory training, and of course, after stopping to hold their breaths all the time.
Hei Kjetil,
Fighting an uphill battle here.. Any chance you have any chronic fatigue syndrome related peer-revived (..) articles?
Thanks,
It is now 2022. I just read this article. It’s fascinating, and I find a lot with which to relate. For decades I have been suffering with what I have called my mystery disease. It is just within the past few months that it has been figured out to be myalgic encephalomyelitis. I am very grateful to it last have a diagnosis. But it is very discouraging that so few people including medical professionals know about this disease in 2022. Especially considering that it has been said that many people with long Covid are developing what can be considered M.E. I would like to know of any other articles and research that you have done that I could read, please. Thank you for all your hard work and considered opinions.
Gratefully and with deep respect,
Mary Redick (Earthsong)
Washington State
Some studies show reduced Cerebral Blood Flow in CFS patients. For example this one: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3139492/
I’m interested in your opinion on these studies. Are these findings consistent with the phenomenon of TOS-CVH and intracranial hypertension, or are these studies flawed in some way?
Great articles! Unfortunately I found it difficult to push the diagnostics towards ICH/CSF leaks. Would you say that there can be a connection between orthostatic hypotension and CSF leaks/intracranial hypertension? In the middle of testing after doing all the rehab from you and a few other specialists. Neck seems to be getting much much better. But headaches are debilitating. Any ideas how to motivate my doctors to refer me for proper testing? Any documented correlation between orthostatic hypotension (no POTS) and the above mentioned?